Pelvic binders
Pelvic binding is an important adjunct in the management of the trauma patient with a suspected “open book” pelvis fracture (AP compression type injury – see pelvis fracture classification below) – correct application can reduce the bony ends of the fracture decreasing pain and bleeding from injured bone cortex. There might be some decrease in venous bleeding as well. In the haemodynamically unstable patient this can result in improved blood pressure.
Note that while binding does reduce the volume of the pelvis, bleeding can still extend into the retroperitoneum if the fracture has disrupted the parapelvic fascia, limiting any tamponade effect that pelvic binding might have.
Young Burgess classification of pelvis fractures
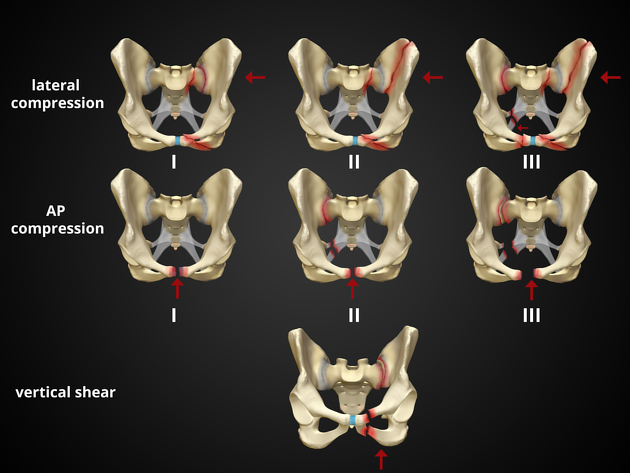
Image courtesy of Dr Matt Skalski, https://radiopaedia.org/ From the case https://radiopaedia.org/cases/37824
Types of binders and application
There are various commercially available pelvic binding devices. The two most commonly used binder in the Northern Region are the “SAM” and the “Prometheus” pelvic splints.
Application technique of the SAM splint can be seen in this video
And application of the Promethus can be viewed in this video
For more detailed information on application – click on this link from St John on Prometheus application
If no binder is available, an improvised device can be fashioned using a sheet tied with towel clips anteriorly.
The binder should remain in place until imaging has been obtained. If there is an open book type injury, the binder should stay on until definitive management is undertaken. It is important that the pubic diastasis is closed radiologically – if not, or if a binder is placed after an initial PXR with this injury, the patient will need to have another PXR to confirm reduction after correct application of the binder.
Patients with lateral compression or anterior shear type injuries will likely not benefit ongoing application of the pelvic binder – however, consult with the orthopaedic team prior to removal.
Related Guidelines
About this guideline
First published: February 2018 (Author: Emma Batistich)
Updated April 2021 (Robert Orec), Sept 2023 (EB), May 2024 (Robert Orec)
Approved by: Northern Region Trauma Network, Health New Zealand | Te Whatu Ora – Northern Region, NRHL, St John
Review due: 2 years