Tension Pneumothorax
Introduction
A tension pneumothorax can occur with blunt or penetrating chest trauma
A laceration to the lung creates a flap-valve – when the patient breathes in, the negative pressure sucks air into the pleural space. The valve traps the air when the patient exhales
The increasing intrathoracic air pushes the mediastinum away from the affected side. This compresses the SVC and IVC leading to decreased venous return causing hypotension and eventually a PEA arrest.
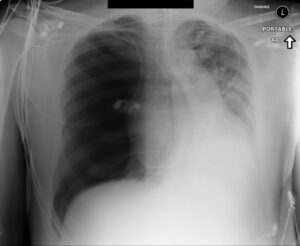
Case courtesy of Dr Andrew Ho, Radiopaedia.org. From the case rID: 23278
Pic 1 – Tension pneumothorax
Clinical signs
- Hypotension
- Tachycardia
- Respiratory distress/Tachypnoea
- Hypoxia
- Subcutaneous emphysema
- Absence of lung sounds on affected side with hyper-resonance to percussion
- Raised JVP*
- Trachea shifted to contralateral side*
*can be difficult to elicit these signs reliably in a trauma patient
Tension pneumothorax is a CLINICAL diagnosis and definitive management in an unstable patient should not be delayed waiting for a CXR
eFAST can be utilised to rapidly confirm clinical suspicions
Management
- Optimise oxygenation
- Consider placing a 14G needle/catheter in the 2nd intercostal space in the midclavicular region (some practitioners may place in the 5th intercostal space in the anterior axilliary line)
- Note: this has a high failure rate, can cause iatrogenic injury and is a temporising measure only – it must be followed up by a formal thoracostomy.
Controversy: needle thoracocentesis for tension pneumothorax
- Perform rapid chest decompression by performing a finger or tube thoracostomy in the 5th intercostal space at the anterior axillary line.
- If the patient is spontaneously breathing, a chest drain must immediately be placed (28-32F drain if patient has a tension pneumothorax)
If the patient remains unstable after insertion of a chest drain to relieve tension pneumothorax, reassess the patient systematically and consider the following:
- Misplaced or kinked tube
- Solution: adjust or replace tube
- Patient has tension pneumothorax on contralateral side
- Solution: decompress contralateral side
- Massive air leak from tracheobronchial injury
- Solution: try placing second tube but patient likely to require thoracotomy
Disposition – interhospital transfer guidelines
tension pthx pdf3
About this guideline
First published: February 2018 (Author: Emma Batistich)
Updated April 2021 (Sue Johnson), May 2024 (Ian Civil)
Approved by: Northern Region Trauma Network, Health New Zealand | Te Whatu Ora – Northern Region, NRHL, St John
Review due: 2 years